Laser treatment of nail fungus
Nail Mycosis
A contagious infection that is caught by walking barefoot...
A proportion of 15% of the French population, constantly increasing, especially adults and seniors is today infected by fungi which ruin the health and appearance of the nails. Its prevalence is 30% after 70 years.
Onychomycosis is caused by dermatophytes (on the feet), yeasts (on the hands) or molds. Foot involvement is the most frequent and the big toe is the main target of dermatophytosis.
Among the dermatophytes it is especially TRICHOPHYTON RUBRUM (73% of cases in the toes and 82% in the fingers) which alters the keratin of the nail.
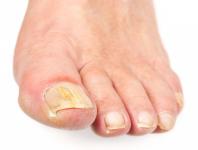
Distolateral subungual onychomycosis is the most common form. It is manifested by subungual hyperkeratosis located at the free edge of the nail plate (inconstantly associated with a white or yellow streak of the plate) with onycholysis (destruction of the nail) by detachment of the nail plate and damage matrix.
The nail is discolored, deformed, thickened, brittle and detaches from the underlying skin.
Common sources of infection include swimming pools, public showers and gyms through contaminated soil.
Transmission is often human-to-human but also geophilic (gardening with open shoes) for dermatophytes.
A person with a fungal infection, who walks barefoot, deposits infected skin fragments on the ground which in turn can transmit the disease. Thus, Trichophyton Rubrum fungi first infect the skin under the feet and between the toes (athlete's foot or Tinea Pedis)
The risk factors are:
Familial predispositions: Some doctors believe that there is a genetic predisposition.
Diseases and drug intake favoring:
• Diseases (AIDS, diabetes, Cushing's syndrome, etc.) or drugs (immunosuppressive treatments, chemotherapy, treatments to prevent transplant rejection, cortisone, etc.) promote infections.
• Disorders of blood circulation (varicose veins in the legs, Raynaud's phenomenon which gives livid extremities in winter).
• Certain genetic diseases such as trisomy 21.
• Skin diseases that lead to detachment or thickening of the nails (psoriasis, lichen planus).
• Foot problems that cause loose and/or thickened nails.
• Toe position abnormalities (overlapping toes, big toes that stick up or “retreat”…)
• Traumas and hematomas caused by sports activities or walking in poorly adapted shoes.
Factors related to lifestyle, occupation and environment
• Humidity, excessive perspiration and continuous wearing of occlusive shoes. Professions where wearing safety shoes or sports shoes is necessary are at high risk for foot fungus. Professions where contact with water and/or food favors hand fungus.
• Walking barefoot on public floors, especially during sports or leisure activities.
Age-related factors
The frequency of nail fungus increases with age, due to the slowing of the nail growth rate but also because of blood circulation disorders.
How do we get this diagnosis?
It is established first of all in front of the clinical aspect and its evolution. This result is confirmed with a nail sample taken by an experienced laboratory. It takes three or four days to find out if it is a mycosis, but about three weeks before being able to identify the causative agent.
What are the standard treatments?
They depend on several factors: the type of fungus and whether or not the nail matrix is affected. If it is not affected, the treatment is usually local: it consists of applying an antifungal varnish for several months; a very restrictive method, often responsible for poor compliance. If the matrix is affected, it is associated with taking an oral antifungal treatment, again, for several months. We obtain 85% of good results, but sometimes at the risk of side effects due to possible hepatotoxicity in some patients, manifested by: digestive or skin disorders... and requires biological monitoring by quarterly blood sampling.
Without treatment, what are the risks?
Spontaneous healing does not exist. Without treatment, the nail deforms more and more, causing aesthetic and even functional discomfort. Above all, it will contaminate others.
The laser is now another solution. What is the latest one, approved by the American health authorities and now used in France?
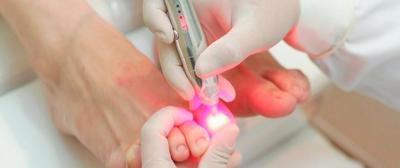
The purpose of the laser is to destroy fungi with a temperature of at least 60°C. This is a thermal effect. The new treatment uses a multi-pulsed laser, the energy of which rises to more than 70°C and which passes through the nail to reach, from below, its bed where the fungus is located. Usually one or two sessions are enough to destroy it. Even if only one nail is affected, the others must be treated.
Is special preparation necessary before a session?
Before the treatment, it is indeed necessary to mill the nails to reduce their thickness to a minimum in order to allow the heat to reach their bed (and to avoid an excessively painful sensation). This new treatment is generally well tolerated, the patient feels some small burns and the transient side effects are manifested by redness around the nail that fades after a few hours.
The main indications for the use of this recent technique by thermal effect?
- We are considering a laser session:
- Referred to by your attending physician or dermatologist.
- In cases of failure of local and oral treatments or when their side effects are too great.
- When patients want a quick, low-cost, side-effect-free solution.
Contraindications are rare (neurological or vascular problems of the feet "Reynaud's syndrome").